In the jungle, any open wound — abrasion, puncture, avulsion, incision, or laceration — is an invitation to infection. To understand infection, and how to tell if you have one, it is helpful to understand the normal process of wound healing, or inflammation.
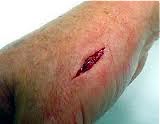 |
| Potential Infection |
When you are cut, the tissue around the wound immediately constricts, compressing the small vessels and slowing blood loss. In fact, for about ten minutes, all the blood vessels in the body reflexively constrict, reducing blood flow even more. Platelets in the blood are attracted to the site of injury and form plugs in the torn vessels. Tissue clotting factors activate the clotting cascade; within minutes, clots of elastic protein fibers fill the wound. This is why, with the aid of direct pressure and elevation, almost all bleeding, even from serious wounds, will stop within ten to fifteen minutes. Over several days, the clot surface dries, forming a natural bandage in the form of a scab.
Underneath the clot, the process of inflammation also forms a protective barrier. After about ten to fifteen minutes, as the clotting process blocks the bleeding from the injured vessels, the body releases vasoactive amines into the wound region, and these cause the uninjured capillaries to get larger and start to leak, so that blood plasma pours into the wound area. In addition, mast cells under the skin release histamine, which attracts white blood cells out of the blood vessels into the extracellular fluid, where they help to clean the wound. Polymorphonuclear granulocytes swallow and kill bacteria; macrophages consume and destroy other debris left lying around.
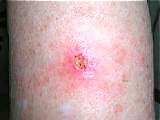 |
| Inflammation |
These processes explain the classical characteristics of acute inflammation, listed mnemonically as four Latin words – rubor, calor, tumor, and dolor. Rubor or redness is due to the dilation of the blood vessels and the escape of red blood cells into the wound area. Calor or heat is also due to vascular dilation and increased local tissue metabolism. Tumor or swelling is caused by the leaking of fluid into the surrounding tissues. Dolor or pain is due to increased tissue tension from fluid accumulation. Some amount of redness, warmth, swelling, and pain are thus part of the normal inflammatory healing process. In addition, a slight temperature elevation is normal for a few days after a severe injury, and lymph nodes in the area of the wound may become mildly enlarged as they help trap bacteria and debris. Again, these signs are normal.
But if the inflammatory process is being overwhelmed by invading bacteria, the body responds by increasing the local inflammation. It is thus excessive inflammation which, among other things, serves as a sign of a local infection.
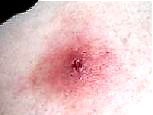 |
| Infection |
- Pain from a wound should normally subside by the second or third day. There may be an infection if pain persists, or especially if the pain increases rather than subsides.
- Redness is usually limited to the margins of a wound, usually within a quarter inch. There may be an infection if the redness extends beyond the margins of the wound. In particular, a clear sign of infection is the presence of red streaks extending from the wound along a limb toward the body.
- Severe swelling may be a sign of infection, especially if the skin temperature increases rather than decreases over time. Increasing limitations of motion, due to swelling and pain, may also indicate an advancing infection.
- Pus is fluid filled with dead white cells. The presence of pus in a wound indicates a failure of cellular defense and confirms the presence of an infection. The pus may be whitish, green, or even reddish, depending on the infecting organism. Sometimes, but not always, there may be a foul odor.
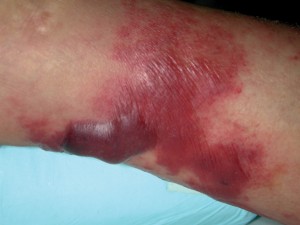 |
| Septicemia |
It is possible for an infection to spread beyond the local area and enter the general blood circulation. This is septicemia, sometimes called blood poisoning. Signs of developing systemic infection include lymphangitis, or enlarged and painful lymph nodes, especially if they are beyond the immediate area of the infection; a high and persistent temperature elevation; chills, headaches, nausea, vomiting, or malaise. A person with a systemic infection is desperately ill and requires immediate evacuation to a facility where definitive care — including intravenous antibiotics — is available.
In any injury, but especially in a wound to the foot, there is particular concern for tetanus, which is caused by Clostridium tetani, an obligate anaerobe that is especially common in soil contaminated with animal feces. All open wounds are susceptible, especially those that have been contaminated with soil. Tetanus is 100 percent fatal, and 100 percent preventable. In my opinion, wilderness leaders and jungle guides should require that all trip participants have up-to-date tetanus booster immunization. A booster shot received shortly after injury may prevent development of the disease.
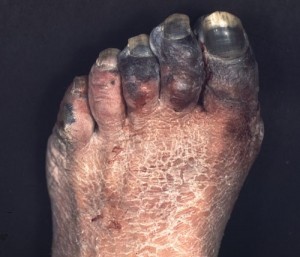 |
| Gangrene |
Gas gangrene results from contamination of a wound by the bacterium Clostridium perfringens, widely found in soil and in the intestinal tracts of humans and animals. The bacteria grow and create spores in dead tissue where the oxygen content is very low. This is why the proper debridement of dead tissue from a wound is extremely important, especially in a wilderness setting. The signs of gangrene include gas bubbles in the wound, drainage of foul-smelling reddish-gray fluid, and crepitus or a “Rice Krispies” feeling in the skin surrounding the wound. The gas bubbles come from the bacteria fermenting carbohydrates into carbon dioxide and hydrogen. Gas bubbles under the skin cause the crepitus. Gangrene is an immediately life-threatening condition, which may be fatal in as little as thirty hours. Immediate evacuation is required.
In the next installment, we will discuss how to prevent and handle infected wounds in the jungle.
- Previous Post: Green Power
- Next Post: The Last Man
- More Articles Related to: Jungle Survival


i have used comfrey root powder to heal bed sores. it works better than anything else i know. have you tried it for jungle sores?
peace and love,
doug highfield