 |
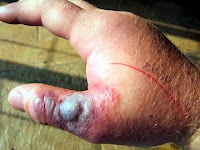
I have written here about the varieties and habits of snakes in the Upper Amazon and how snakebite is treated by local healers. Remember, of course, that your chance of being bitten by a venomous snake in the Amazon is really very small, especially if you take basic precautions, such as not sticking your hand blindly into places where a snake might be sleeping. It is probably worth noting that more than fifty percent of pit viper envenomations in North America are associated with alcohol ingestion on the part of the victim.
There are, as I said, two families of venomous snakes in the Upper Amazon — the Crotalidae or pit vipers and the Elapidae or coral snakes. If you are bitten by a pit viper — and actually envenomated — you are in for a memorably unpleasant experience. But, if you treat the wound properly and avoid infection, you are unlikely to die or have permanent injuries.
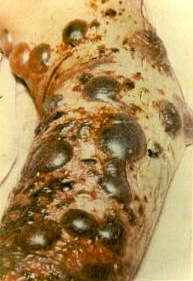 |
There is no question that a Crotalid envenomation is a medical emergency requiring urgent evacuation, if at all possible, to a definitive care facility that is equipped to administer Crotalid antivenom. In an ideal world, anyone envenomated by a pit viper in the wilderness would be immediately evacuated and receive antivenom within four hours — six at the most — in a hospital setting, under sterile conditions, with constant monitoring, and with a crash cart available in case of an allergic reaction. If such an evacuation is possible, then by all means it should be done. As professional handlers of venomous snakes say, “The best equipment for treating a venomous snakebite is a set of car keys.”
However, the first step in treatment is to avoid panic. Death is rare. Even without evacuation, most cases result in several days of serious misery and then full recovery. Remember that the fatality rate even for untreated pit viper bites is extremely low. The treatment steps are:
- Use the Sawyer Extractor. If you are in snake country, the Extractor should always be within easy reach in your pack. The Extractor can remove as much as 30 percent of Crotalid venom proteins if applied within three minutes. Use the Extractor as quickly as possible and then keep it on the bite for about thirty minutes. Because of the great suction it creates, no cutting is necessary. This should always be the first thing you do, even when evacuation is in progress.
- Remove rings, bracelets, or any other constricting jewelry on the affected limb, which may swell to as much as twice its normal size.
- Immobilize the bitten extremity with a splint, just as you would a fracture.
- Have the patient rest and keep activity to a minimum.
- Have the patient drink as much fluid as possible, in frequent small amounts, in order to maintain fluid volume and kidney flow.
- Remember that a snakebite is a contaminated puncture wound, and treat it as such.
- Get to definitive care as quickly as you can. Otherwise, have the patient rest and drink fluids; keep the wound clean; give lots of encouragement and support.
The following are not recommended for pit viper envenomations:
 |
- Do not make incisions or try to suck out the venom. In jungle conditions, cutting into an already compromised limb is asking for an infection. You absolutely do not want pit viper venom in your mouth. Conversely, your mouth is full of all kinds of bacteria. And you can’t suck as hard as the Extractor can anyway.
- Do not use a tourniquet. Tourniquets can result in loss of the limb due to decreased blood flow. In addition, you are just keeping the venom localized where it does the most tissue damage.
- Do not use electric shock. It can be dangerous, and has no proven value in managing pit viper bites. It is the great urban legend of wilderness first aid.
- Do not use ice. There is no evidence that snake venom enzyme activity diminishes with cold. Freezing already compromised tissue can lead to frostbite, which can damage the limb more than the original bite. Packing in ice has probably resulted in more lost limbs than snakebite itself; this is particularly tragic when limbs have been lost to frostbite because of a non-envenomated bite.
- Do not give alcohol. It causes vessels to dilate and may speed venom absorption.
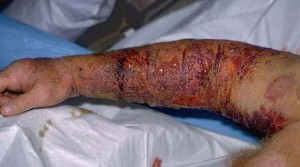 |
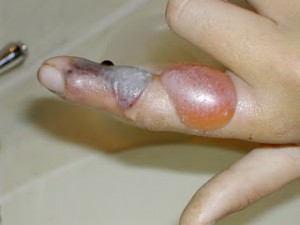
The use of an elastic bandage pressure wrap — recommended for use with bites from Elapidae or coral snakes — has been recommended for use in some cases of Crotalid envenomation as well. The argument against its use is that the pressure may actually increase the risk of disfiguring local tissue damage, which may then require skin grafts and extensive repair and treatment; and that removal of the pressure may result in sudden massive swelling and discoloration. The argument in favor of its use is that the spread of venom to vital organs can be life-threatening — in fact, some Crotalid bites can cause serious damage to limbs even when the bites were to a finger or foot — and the use of a pressure bandage can prevent this spread, even at the risk of greater localized damage. The way to apply a pressure bandage is described here.
The problem is that there is no way of knowing how serious the envenomation is at the outset, when the decision must be made. There is a tradeoff between averting more serious life-threatening damage and increasing the risk of painful and disfiguring local damage. Such a decision should be considered a serious one, to be decided in full consultation with the patient.
- Previous Post: The Psychedelic Review
- Next Post: Dealing with Snakebite II
- More Articles Related to: Jungle Survival


thatz so cool but itz so sad at da same time i hope that they never get biten again
I agree. I hope they never get bitten again too.