Someone carelessly tossed a machete in the bottom of the boat, your barefoot friend stepped on it, and now he has a laceration that is bleeding all over the place. Do not panic. Here are the steps to take.
Step 1. Protect yourself. The first step in wound care is to protect yourself from blood-borne pathogens, including HIV and Hepatitis B.
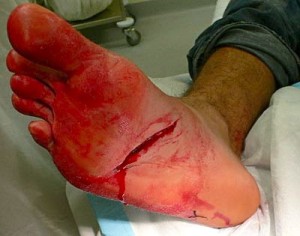 |
| Bare foot meets carelessly tossed machete |
![]() Always assume that all body substances are infectious.
Always assume that all body substances are infectious.
![]() Wash your hands before and after any wound contact, either with soap and water or — even better — an alcohol gel, such as those made by Purell or Lysol.
Wash your hands before and after any wound contact, either with soap and water or — even better — an alcohol gel, such as those made by Purell or Lysol.
![]() Carry some exam gloves in your medical kit, and put them on for any anticipated contact with nonintact skin, blood, body fluids, mucous membranes, or contaminated items. Wash your hands immediately after you remove the gloves.
Carry some exam gloves in your medical kit, and put them on for any anticipated contact with nonintact skin, blood, body fluids, mucous membranes, or contaminated items. Wash your hands immediately after you remove the gloves.
![]() Protect your own mucous membranes — eyes, nose, and mouth — from blood splash. Tie a bandana around your face, and put on your glasses.
Protect your own mucous membranes — eyes, nose, and mouth — from blood splash. Tie a bandana around your face, and put on your glasses.
Step 2. Stop the bleeding. The second step in wound care is to stop further blood loss. Apart from an obstructed airway, nothing else matters until the flow of blood is stopped.
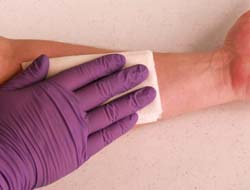 |
| Apply direct pressure on the wound to stop bleeding |
![]() In almost every case — even in amputations — bleeding can be stopped by elevating the wound above the level of the heart and applying strong direct pressure for about ten to fifteen minutes. Blood is slippery, so use a piece of gauze, preferably sterile, or even a clean bandana if that is all you have; a Kotex pad tossed in your medical kit is ideal for this purpose. Put your thumb or fingers or your whole palm over the wound and press down hard; alert and cooperative patients can do this themselves. If the gauze gets soaked with blood, do not remove it, but add more gauze.
In almost every case — even in amputations — bleeding can be stopped by elevating the wound above the level of the heart and applying strong direct pressure for about ten to fifteen minutes. Blood is slippery, so use a piece of gauze, preferably sterile, or even a clean bandana if that is all you have; a Kotex pad tossed in your medical kit is ideal for this purpose. Put your thumb or fingers or your whole palm over the wound and press down hard; alert and cooperative patients can do this themselves. If the gauze gets soaked with blood, do not remove it, but add more gauze.
![]() Do not use a tourniquet. Tourniquets kill limbs. There may be occasions when a tourniquet is necessary, such as massive shrapnel wounds, but using a tourniquet is a deliberate decision to sacrifice a limb in order to save a life.
Do not use a tourniquet. Tourniquets kill limbs. There may be occasions when a tourniquet is necessary, such as massive shrapnel wounds, but using a tourniquet is a deliberate decision to sacrifice a limb in order to save a life.
Step 3. Clean the wound. The third step in wound care — especially in the jungle — is to make sure the wound is as clean as you can possibly make it.
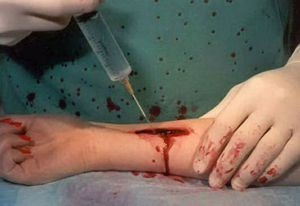 |
| Clean the wound with an irrigation syringe … |
![]() Remove any existing bandages or wound closure strips.
Remove any existing bandages or wound closure strips.
![]() Clean the skin around the wound with soap and water or a topical antiseptic such as povidone iodine. Scrub gently with a sterile gauze pad. The idea is to remove any dirt that might seed the wound with bacteria. Avoid getting soap or antiseptic in the wound itself. Scrub in a spiral pattern away from the wound rather than toward it.
Clean the skin around the wound with soap and water or a topical antiseptic such as povidone iodine. Scrub gently with a sterile gauze pad. The idea is to remove any dirt that might seed the wound with bacteria. Avoid getting soap or antiseptic in the wound itself. Scrub in a spiral pattern away from the wound rather than toward it.
![]() Allow the wound to open naturally. If necessary, spread the wound edges apart using a pair of sterile forceps.
Allow the wound to open naturally. If necessary, spread the wound edges apart using a pair of sterile forceps.
![]() If the wound has become infected, pus has probably collected in pockets, so gently probe the deeper parts of the wound with a sterile instrument to make sure that all such pockets are drained.
If the wound has become infected, pus has probably collected in pockets, so gently probe the deeper parts of the wound with a sterile instrument to make sure that all such pockets are drained.
![]() Irrigate the wound copiously with a high-pressure stream of purified water to remove clotted blood, pus, debris, and other contaminants. Use an irrigation syringe and splash shield; in an emergency, you can use any sort of clean plastic bag with a pinhole punched in it, or melt a pinhole in the top of a standard water bottle, but protect yourself from blood splash.
Irrigate the wound copiously with a high-pressure stream of purified water to remove clotted blood, pus, debris, and other contaminants. Use an irrigation syringe and splash shield; in an emergency, you can use any sort of clean plastic bag with a pinhole punched in it, or melt a pinhole in the top of a standard water bottle, but protect yourself from blood splash.
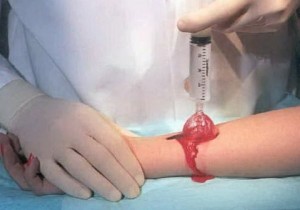 |
| … preferably one with a splash shield |
![]() The primary medium for infection within a wound is dead tissue. Dead tissue is basically meat. It has no blood supply; white cells and antibodies have difficulty penetrating it; and thus it is a good culture medium for bacteria and fungi. You can identify living tissue because it is reddish, elastic, and bleeds when you poke it; dead tissue is dark, mushy, and does not bleed. Look for dead tissue in the wound. If any remains after high-pressure irrigation, then — unless a relatively brief evacuation is imminent — it must be removed or debrided. In a wilderness emergency situation, your best bet is to scrub the wound with sterile sponges, sterile dressings, or sterile pieces of cotton. Rough cloth works better than smooth cloth. Scrub with firmness. It will hurt. Your friend will use very bad language. The wound will bleed again, since clots will have been knocked off, but the bleeding can readily be stopped by direct pressure with a sterile dressing.
The primary medium for infection within a wound is dead tissue. Dead tissue is basically meat. It has no blood supply; white cells and antibodies have difficulty penetrating it; and thus it is a good culture medium for bacteria and fungi. You can identify living tissue because it is reddish, elastic, and bleeds when you poke it; dead tissue is dark, mushy, and does not bleed. Look for dead tissue in the wound. If any remains after high-pressure irrigation, then — unless a relatively brief evacuation is imminent — it must be removed or debrided. In a wilderness emergency situation, your best bet is to scrub the wound with sterile sponges, sterile dressings, or sterile pieces of cotton. Rough cloth works better than smooth cloth. Scrub with firmness. It will hurt. Your friend will use very bad language. The wound will bleed again, since clots will have been knocked off, but the bleeding can readily be stopped by direct pressure with a sterile dressing.
![]() Always follow any debridement with additional high-pressure irrigation. The wound should be clean and pink.
Always follow any debridement with additional high-pressure irrigation. The wound should be clean and pink.
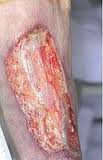 |
| A cleaned and debrided wound |
Step 4. Protect the wound. Once the wound is cleaned of dirt, debris, pus, and dead tissue, the fourth step is to dress the wound to provide a healing environment and prevent further contamination.
![]() A dressing is any material applied to a wound to control bleeding and prevent contamination; a bandage is any material used to hold a dressing in place. Think about dressings and bandages in layers. Immediately next to the skin should be a nonadherent base — Telfa, Second Skin, Xeroform, a piece of sterile gauze impregnated with petroleum jelly — that will not stick to the wound. Above that should be a gauze sponge to absorb wound discharge. Those two layers should be held in place by bandaging material that either sticks to itself or is attached to the skin with adhesive tape.
A dressing is any material applied to a wound to control bleeding and prevent contamination; a bandage is any material used to hold a dressing in place. Think about dressings and bandages in layers. Immediately next to the skin should be a nonadherent base — Telfa, Second Skin, Xeroform, a piece of sterile gauze impregnated with petroleum jelly — that will not stick to the wound. Above that should be a gauze sponge to absorb wound discharge. Those two layers should be held in place by bandaging material that either sticks to itself or is attached to the skin with adhesive tape.
![]() Dressings and bandages are often sold as a combined adhesive wound covering. A simple Band-Aid is a good example — neat, versatile, and sterile.
Dressings and bandages are often sold as a combined adhesive wound covering. A simple Band-Aid is a good example — neat, versatile, and sterile.
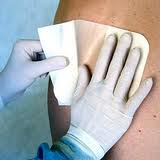 |
| Apply a dressing … |
![]() If you were not in the middle of the jungle, it might make sense to use butterfly strips or Dermabond tissue adhesive to bring the edges of the wound together and minimize scarring. But closing the edges of a wound can create a deep dark warm pocket in which bacteria can grow and form an abscess. At this point, avoiding an abscess should be a higher priority than minimizing a scar.
If you were not in the middle of the jungle, it might make sense to use butterfly strips or Dermabond tissue adhesive to bring the edges of the wound together and minimize scarring. But closing the edges of a wound can create a deep dark warm pocket in which bacteria can grow and form an abscess. At this point, avoiding an abscess should be a higher priority than minimizing a scar.
![]() A goal of the dressing is to keep the wound moist and create an environment that encourages healing. Current nonadherent dressing materials — including sterile gauze impregnated with petroleum jelly — are designed to provide such an environment. You can also apply a thin layer of antibiotic ointment, which helps keep the wound moist, and may — or may not — provide some additional protection from infection. Bear in mind that no amount of antibiotic ointment can compensate for inadequate wound cleaning.
A goal of the dressing is to keep the wound moist and create an environment that encourages healing. Current nonadherent dressing materials — including sterile gauze impregnated with petroleum jelly — are designed to provide such an environment. You can also apply a thin layer of antibiotic ointment, which helps keep the wound moist, and may — or may not — provide some additional protection from infection. Bear in mind that no amount of antibiotic ointment can compensate for inadequate wound cleaning.
![]() Antibiotic ointments designed for wound care usually combine antibiotics effective against both gram-positive and gram-negative bacteria. The antibiotic bacitracin targets gram-positive bacteria; neomycin and polymyxin target gram-negative bacteria. Triple antibiotic ointments — brand names include Neosporin and Mycitracin — contain all three. However, some people have allergic skin reactions to neomycin, so some antibiotic ointments, such as Polysporin, contain just bacitracin and polymyxin, which provide the same coverage. Some antibiotic ointments add the topical analgesic pramocaine. Check the ingredients before you buy.
Antibiotic ointments designed for wound care usually combine antibiotics effective against both gram-positive and gram-negative bacteria. The antibiotic bacitracin targets gram-positive bacteria; neomycin and polymyxin target gram-negative bacteria. Triple antibiotic ointments — brand names include Neosporin and Mycitracin — contain all three. However, some people have allergic skin reactions to neomycin, so some antibiotic ointments, such as Polysporin, contain just bacitracin and polymyxin, which provide the same coverage. Some antibiotic ointments add the topical analgesic pramocaine. Check the ingredients before you buy.
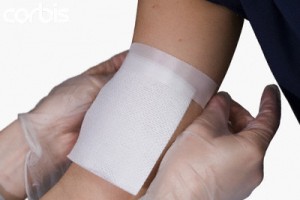 |
| … and bandage |
![]() If you are applying a dressing with a separate bandage, try to avoid wrapping the bandage or adhesive tape completely around a limb. It can obstruct circulation, like a tourniquet, as the limb swells. If you must wrap a limb, monitor the distal pulses and check frequently for bluish color, tingling, or loss of sensation.
If you are applying a dressing with a separate bandage, try to avoid wrapping the bandage or adhesive tape completely around a limb. It can obstruct circulation, like a tourniquet, as the limb swells. If you must wrap a limb, monitor the distal pulses and check frequently for bluish color, tingling, or loss of sensation.
![]() Movement may cause bleeding to recur, so severely injured limbs should be immobilized before evacuation. Elevation of an infected wound can reduce swelling and pain.
Movement may cause bleeding to recur, so severely injured limbs should be immobilized before evacuation. Elevation of an infected wound can reduce swelling and pain.
Step 5. Watch the wound. The fifth step in wound care is to change the dressing periodically and examine the wound carefully.
![]() Be alert for signs of infection.
Be alert for signs of infection.
![]() Infected wounds should be drained and washed, as described above, two or three times a day.
Infected wounds should be drained and washed, as described above, two or three times a day.
![]() Infected wounds benefit from warm compresses for 15 to 20 minutes several times a day. The warmth causes the blood vessels to dilate, increases blood flow to the area, helps the body fight the infection, and loosens clots, scabs, dried serum, and pus. For an injury to a finger or toe, it is possible to immerse the wound in warm, sterile water to which an antiseptic such as povidone iodine has been added. You can make a hot compress by bringing a piece of cloth to a boil in water to make it hot and sterile, then wringing it out, folding it, and placing it against the wound.
Infected wounds benefit from warm compresses for 15 to 20 minutes several times a day. The warmth causes the blood vessels to dilate, increases blood flow to the area, helps the body fight the infection, and loosens clots, scabs, dried serum, and pus. For an injury to a finger or toe, it is possible to immerse the wound in warm, sterile water to which an antiseptic such as povidone iodine has been added. You can make a hot compress by bringing a piece of cloth to a boil in water to make it hot and sterile, then wringing it out, folding it, and placing it against the wound.
Step 6. Consider evacuation. Once you have done everything you can to clean and protect the wound, the sixth step in wound care is to consider whether the wound is beyond your skill and requires evacuation to definitive care. Seriously consider evacuation in cases of
![]() Severe animal bites, especially from potentially rabid animals
Severe animal bites, especially from potentially rabid animals
![]() Deep puncture wounds, dirty wounds with embedded foreign material, and wounds that contain crushed, shredded, or ragged tissue, where there is high risk of infection
Deep puncture wounds, dirty wounds with embedded foreign material, and wounds that contain crushed, shredded, or ragged tissue, where there is high risk of infection
![]() Wounds involving joints, severed tendons, or fractures
Wounds involving joints, severed tendons, or fractures
![]() Infected wounds that do not respond promptly to treatment
Infected wounds that do not respond promptly to treatment
![]() Severe blood loss
Severe blood loss
- Previous Post: Bioneers
- Next Post: Sacred Justice, Part 1
- More Articles Related to: Jungle Survival


Hi Steve,
Thanks for another informative post. As essential as a machete can be in saving our life, it can easily be our undoing. Your post also raises some interesting questions about exactly what we should be carrying in our packs when travelling through the jungle. I’d be really interested to hear your thoughts.
Regards,
Leon.
Leon —
Thank you for your comment. I have been wondering whether anyone has been reading the jungle survival tips — after all, they have little to do with shamanism — and whether they have been helpful, so it is good to hear from you. You raise a valuable point, and you have tempted me to do a blog post on the subject.
Just briefly, though, I think it is very easy to get stuff-oriented when thinking about survival skills, when it is much better to be knowledge- and skills-oriented. So, in answer to your question: the best thing to carry with you in the jungle is a certification card from a good course in wilderness first aid. :-)
I will expand on that in another post.
My friends love your survival info. Keep it coming.
Hi! Thank you for info on infections and some gory pictures:-). I had a cut last summer, in the middle of the city:-). I left it alone and I didn’t have it looked at. But after a couple of days, I put some (old, non-sterile it turned out) Aloe Vera on the crust. Another few days later an infection broke out, stinging, dark red skin and all. At the emergency room they cleaned the wound precisely like you say, and, yes, it hurts near the surface/skin, but not inside the flesh. And they put me on an antibiotic and stressed the importance of taking it.
But it sounds like you are saying that an infection is not necessarily a death sentence, even if you don’t take antibiotics. Are you saying that with good cleaning and ideal conditions, you could probably fight an infection?
In the future, I would love to see an article about available healing plants and their use in this context. If you travel and get hurt, there is always some old native who comes over with some old wive’s tale about what to do. I met one in Greece who insisted on putting regular tobacco on the wound, but it was a very shallow wound and went ok. How trustworthy are local curanderos in this regard?